New Year, Same Pandemic
The turn of the year has come and gone but a lot of the news feels the same in year two of the COVID19 pandemic. Many countries are experiencing severe 2nd and 3rd waves of infection. Highly transmissible new variants of the virus cast a cloud on the excitement and hope brought by effective new vaccines. COVID19 has become a part of daily life as a mask weary society trudges along, numb to the rising global death count.

When does it end? How does in end? When can we get back to life as we once knew it? I get these questions often and wish I had good answers. Effective vaccines are a light at the end of the tunnel but in an unequal world, how close that light feels and how brightly it shines depends on where you find yourself. As a frontline health worker in the United States, I was privileged to be among the first to receive the Pfizer mRNA vaccine. My absolute joy and relief at being immunized are tempered by the uncertainty that surrounds when my parents, will be able to access these live-saving vaccines. Like many others living in resource poor countries, for my parents the projections for access to COVID19 vaccines are bleak. It is estimated that at least 85 poor countries will not have widespread access to COVID19 vaccination before 2023, year 4 of the pandemic !!!

Effective Vaccines, Amplified Inequity
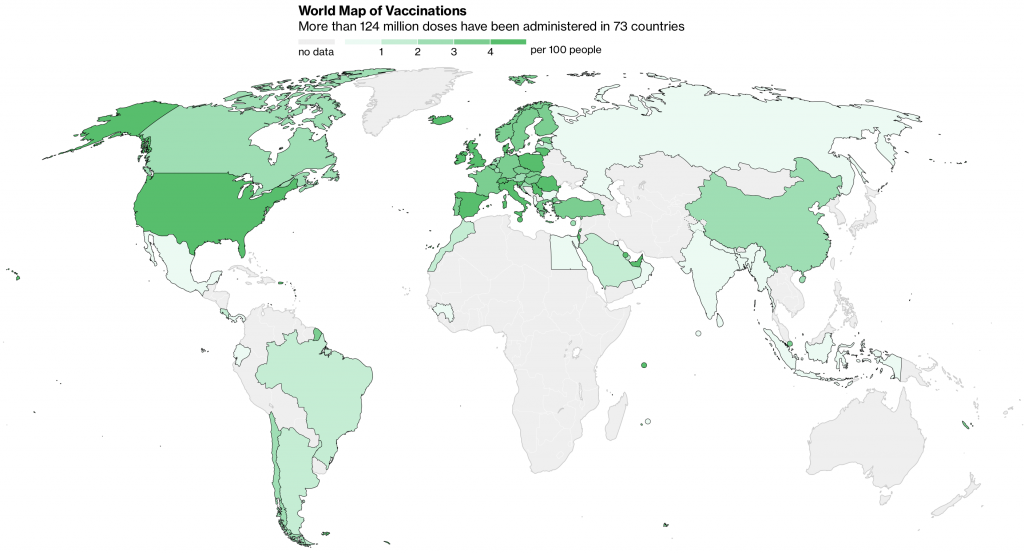
It is a feat of science that in just over a year since SARSCoV2 was identified, we now have 10 effective vaccines being deployed around the globe. Inequity has sadly been a central feature of this pandemic affecting access to protective equipment, diagnostics and treatment and now vaccines. At the current global vaccination rate of 4,607,324 doses a day it would take an estimated 6.8 years to vaccinate 75% of the world’s population. The world’s poorest and most vulnerable find themselves at the tail end of the global queue for COVID19 vaccination. 124 million vaccine doses have been delivered in 73 countries of which 4,935,611 doses (4%) in South America and a paltry 446,904 doses (0.37%) in Africa. The 20 wealthiest countries have the lion’s share representing 80% of the vaccine doses delivered so far.
COVAX – Bringing the World Together
The COVAX initiative co-led by WHO, GAVI and CEPI provides a risk-sharing mechanism for pooling resources to procure and equitably distribute COVID19 vaccines to countries regardless of wealth. It aims to deliver enough vaccine doses to allow participating countries to immunize 20% of their populations by the end of 2021. This goal is ambitious but the urgency of the moment demands it. To achieve this target, COVAX will have to raise an additional $6.8 billion in 2021 – $800 million for research and development, $4.6 billion for acquiring doses and $1.4 billion for delivery support. Its success largely depends on effective fundraising and donors making good on their pledges. The recent news that COVAX will ship 90 million doses of vaccine to Africa starting in February of 2021 is a welcome start. Put in perspective, these doses will cover about 3% of the continent’s 1.3 billion strong population. COVAX is doing a lot but it cannot do it all alone. Important regional and national efforts to bolster vaccine access for poor countries have to contend with a tense and competitive vaccine market as well as vaccine nationalism.

Vaccine Nationalism – An Existential Threat
So far in the pandemic, countries have prioritized their own populations instead of a more concerted global effort working together to defeat the virus. This has been reflected in international trade restrictions which in the early days of the pandemic severely hampered the ability of poorer countries to respond effectively. The ongoing dispute on vaccine access and rollout between the EU and the UK is just the latest illustration of this. With many vaccine manufacturers experiencing delays in production and failing to meet delivery targets, the shortfall led the EU to impose export restrictions on COVID19 vaccines produced within the bloc. Although the EU has since backtracked on the widely condemned decision, the words of the EU commission
“The protection and safety of our citizens is a priority and the challenges we now face left us with no choice but to act,”
raise alarm bells that more countries will impose vaccine export bans to protect their own supplies. Poorer countries already struggling for access to vaccines will bear the brunt of the fall out.
Similar scenarios have played out in very recent history. In 2009 during the H1N1 influenza outbreak which killed 284,000 people globally, a vaccine was developed in just 7 months. However almost all of the vaccine supplies were hoarded by wealthy countries leaving others with nothing. The same can be said about eradication programs for smallpox and polio, for which vaccines only became widely available to the world’s poorest when these diseases had been largely eradicated from richer parts of the world.
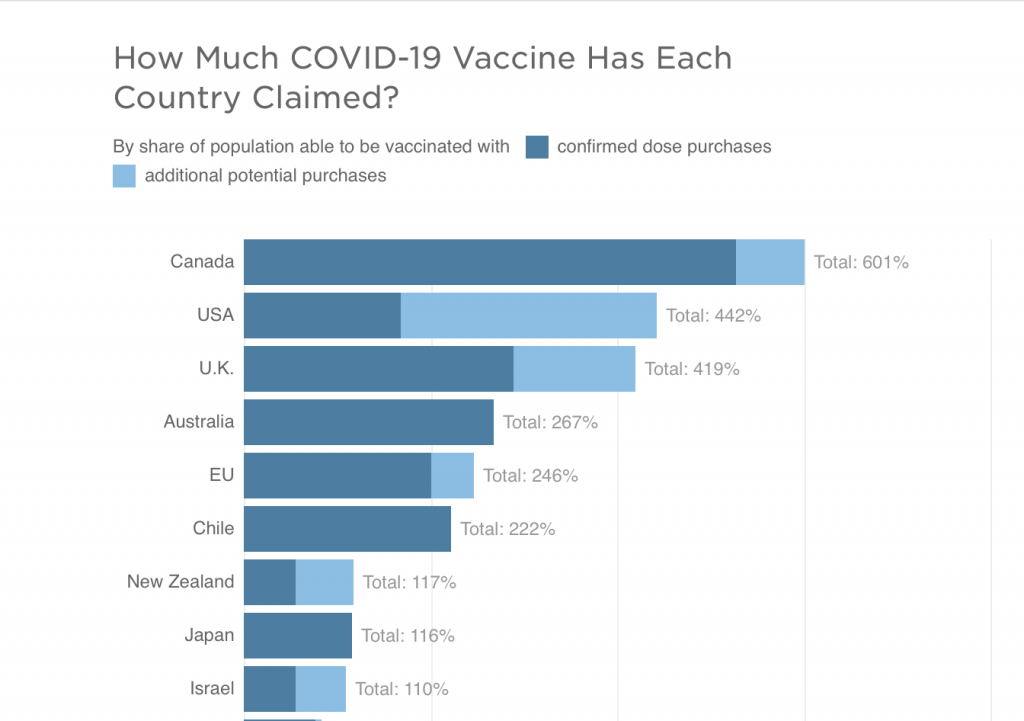
Source: Launch and Scale Speedometer, Duke Global Health Innovation Center
Credit: Connie Hanzhang Jin/NPR
The Case for Acting Now and Acting Fast
The cost of inaction on global vaccine inequity is the risk of seeing COVID19 become just another in a long list of diseases which primarily affect the poor. Unlike Malaria, Tuberculosis and HIV, the world will not be able to “move on” if the problem is not confronted simultaneously on all fronts. The estimated monthly financial cost of the pandemic to the global economy is a staggering $375 billion. Besides the moral imperative to act, the financial arguments are equally compelling.

VAXXING TO SAVE Economies
A recent study commissioned by the international chamber of commerce projects that in a worse case scenario in which wealthiest countries are fully vaccinated by the middle of this year and poor countries are completely left out, the global economy could see losses exceeding $9 trillion! In the more likely scenario in which most wealthy countries could vaccinate 70-80% of their populations by the end of the 2021, the projected losses will still fall in the $1.8-$3.8trillion range. A significant proportion of these losses will be borne by wealthy countries, especially those heavily reliant on trade. In an interconnected world with global supply chains, sharing vaccines is more than just charity. In essence, the economic recovery of the strongest and the weakest economies are intimately connected to controlling the spread of the virus globally.

Emerging variants and the race to vaccinate
Emerging variants of SARSCoV2 present a new challenge and have brought a sense of enhanced urgency to accelerate the distribution of vaccines. Some of the more concerning variants have accumulated changes in the genome of the virus which make them more transmissible and easier to spread. In addition there is growing evidence that some of the changes in the virus genome could compromise the efficacy of first generation vaccines and antibody-based therapies. Many countries in sub-saharan Africa are seeing a surge of cases and deaths fueled by the spread of these new variants. Between December 29th 2020 and January 25th, 2021, new infections on the continent rose by 50% when compared to the preceding four weeks. The region had successfully weathered relatively milder first waves of the pandemic compared to other regions, by relying mainly on rigorous public health mitigation.

The collision of COVID19 fatigue, substantial economic losses from lockdowns and more transmissible variants creates a perfect storm. Severe subsequent waves of the virus could quickly overwhelm fragile health systems and be the deadliest yet. South Africa, where the 501Y-V2 variant of the virus was first identified, is experiencing its worse pandemic surge with massive case spikes, overwhelmed hospitals and a rising death toll. For weak healthcare systems with limited human and material resources, providing vaccination to frontline workers at the minimum is vital to preserving a functioning healthcare system. This is especially important in lower income countries where the pandemic has already severely impacted gains in other priority areas of global health including; access to HIV treatment, Polio eradication, Tuberculosis Control and Malaria prevention.
COVID DENIALISM AND Vaccine hesitancy – The ElephantS in the room
Vaccine hesitancy and COVID19 denialism are important and concerning threats which must be confronted and addressed in tandem with ensuring access to vaccines for all. Effective vaccines will only help if these can be delivered to those who need them the most. The current situation in Tanzania, has garnered international attention with its government openly shunning mask mandates and lockdowns and now rejecting COVID19 vaccines. Burundi, has also opted out, stating its intention to focus efforts more towards mitigation than mass immunization. Brazil which has experienced one of the worse outbreaks of COVID19 was largely crippled in its response by leadership which also shunned containment measures and vaccination. Even in countries willing to accept vaccine doses, there is considerable hesitancy within the populations which could significantly compromise vaccine distribution. The same fervor that is being applied to sourcing vaccines, must also be directed at increasing uptake. Aggressive information and education campaigns as well as incentives which have proven useful for other epidemics must serve as lessons. Confronting government sponsored vaccine denialism is more challenging because every country has the autonomy to define its internal health policy, even if these policies are harmful to its own citizens.
Where DO We GO FROM HERE?

Despite the isolation of the pandemic, the world strangely feels more connected through our shared trauma from the losses we have experienced and the changes in our daily lives. Effective vaccines provide hope for better days ahead and our collective humanity demands that we ensure this hope is felt by all. No country is an island in a global pandemic and making it out together also means bringing along those who need a little extra help on the road.